Considering a hair transplant is a significant decision for many individuals experiencing hair loss. While it offers a promising solution, it’s crucial to understand that certain pre-existing health conditions can influence candidacy and the overall success of the procedure. This comprehensive guide delves into how chronic conditions such as psoriasis, the use of antidepressants, and the presence of keloids can affect your eligibility for a hair transplant.
Key Considerations for Hair Transplant Candidacy with Chronic Conditions:
- Scalp Health Assessment: Evaluating the condition of your scalp is paramount.
- Medication Interactions: Understanding how current medications might affect healing and results.
- Scarring Tendencies: Assessing the risk of abnormal scarring and its impact.
- Surgical Risks: Identifying potential complications related to your specific condition.
- Long-Term Management: Planning for post-operative care and potential condition management.
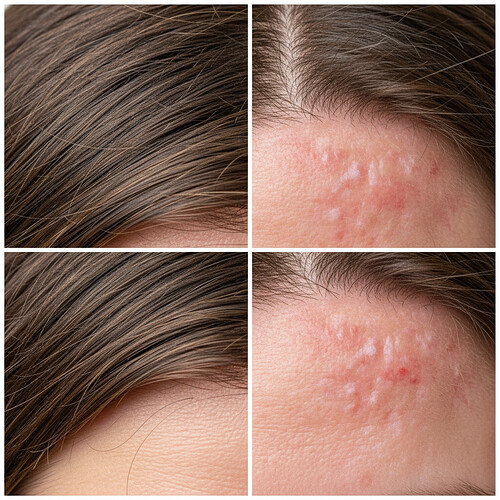
Understanding Psoriasis and Hair Transplants
Psoriasis is a chronic autoimmune condition characterized by red, itchy, scaly patches, most commonly on the scalp. When considering a hair transplant, active scalp psoriasis presents a significant challenge. The inflammation and irritation associated with psoriasis can compromise the healing process of the scalp after the procedure. Furthermore, the areas affected by psoriasis may not be ideal for graft implantation, as the condition can impact the viability of transplanted hair follicles.
Impact of Psoriasis:
- Inflammation: Active inflammation can impede the healing of both donor and recipient sites.
- Graft Survival: The inflammatory environment may reduce the survival rate of transplanted grafts.
- Scarring: Psoriatic plaques can sometimes lead to scarring, potentially affecting aesthetic outcomes.
- Medication: Topical or systemic treatments for psoriasis might interfere with post-transplant medications or healing.
Candidacy with Psoriasis:
Individuals with well-controlled, inactive scalp psoriasis may still be considered candidates for a hair transplant. However, a thorough consultation with both a dermatologist and the hair transplant surgeon is essential. The surgeon will need to assess the extent and severity of the psoriasis, determine if the condition is currently flaring, and discuss potential risks. In some cases, it might be recommended to achieve remission of psoriasis before proceeding with the transplant. The surgeon may also advise on specific techniques or graft harvesting methods that minimize trauma to the scalp. Post-operative care will also need to be carefully managed to avoid exacerbating the psoriasis.
The Influence of Antidepressants on Hair Transplants
Antidepressants are commonly prescribed medications used to treat depression and other mental health conditions. While not directly affecting the hair follicles, some antidepressants can have indirect implications for hair transplant surgery. The primary concern revolves around their potential impact on healing and the risk of side effects that could interfere with the recovery process.
Potential Concerns with Antidepressants:
- Blood Thinning Effects: Certain antidepressants, particularly SSRIs (Selective Serotonin Reuptake Inhibitors), can have mild blood-thinning properties. This could theoretically increase the risk of bleeding during and after the procedure, although this is generally considered a minor risk for most patients.
- Healing Process: Any medication that affects the body’s overall physiological state could potentially influence wound healing. However, most modern antidepressants are not known to significantly impair wound healing in the context of a hair transplant.
- Drug Interactions: It’s crucial to inform your surgeon about all medications you are taking, including antidepressants. They can assess potential interactions with anesthetic agents or post-operative medications.
Candidacy with Antidepressants:
In most cases, being on antidepressants does not disqualify you from undergoing a hair transplant. The key is transparency. Patients must disclose their full medical history and all medications to their surgeon. The surgical team will then evaluate the specific antidepressant, dosage, and the patient’s overall health. If there are concerns about blood thinning, the surgeon might recommend adjusting the dosage or temporarily stopping certain medications under the guidance of the prescribing physician. However, abruptly stopping antidepressant medication can have severe consequences, so this decision must be made in consultation with a mental health professional and the surgical team. The focus remains on ensuring the patient’s safety and optimizing the healing environment.
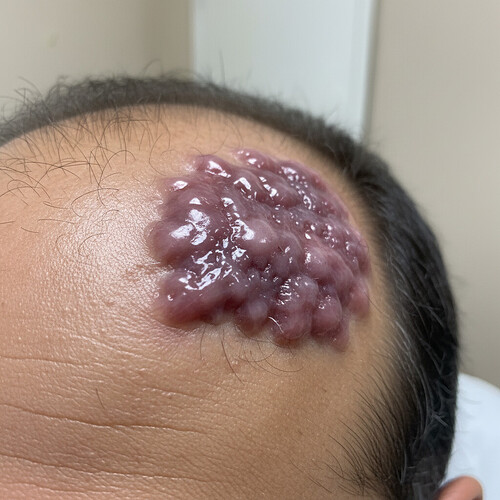
Keloids and Hair Transplant Surgery
Keloids are raised, often itchy, scars that grow beyond the boundaries of the original wound. They are a result of an overactive healing response. Individuals prone to developing keloids, especially after minor injuries or surgery, need to be particularly cautious when considering a hair transplant.
Risks Associated with Keloid Tendency:
- Donor Site Scarring: The most significant concern is the potential for keloid formation at the donor site, particularly in Follicular Unit Transplantation (FUT) procedures, which involve a linear incision. While Follicular Unit Extraction (FUE) minimizes scarring, keloid tendencies can still manifest, albeit often less prominently.
- Recipient Site Scarring: Although less common, keloids can also form at the recipient sites where individual follicular units are implanted.
- Aesthetic Concerns: Visible keloids on the scalp can be cosmetically undesirable and may outweigh the perceived benefits of the hair transplant.
Candidacy with Keloid Tendencies:
Individuals with a known history of keloid formation are often considered higher-risk candidates for hair transplant surgery. The surgeon will carefully assess the patient’s medical history, including any previous surgeries and their outcomes. If a patient has a history of keloids, the surgeon might recommend:
- FUE over FUT: Preferring the FUE technique due to its less invasive nature and smaller, more scattered potential scarring.
- Smaller Sessions: Performing the procedure in smaller, more manageable sessions to monitor healing.
- Preventative Measures: Discussing potential preventative strategies, such as using silicone sheets or specialized creams post-operatively.
- Alternative Solutions: In severe cases, the surgeon might advise against the procedure altogether or suggest alternative treatments for hair loss that do not involve invasive surgery. A consultation with a dermatologist experienced in scar management can also be beneficial.
`
Conclusion: A Personalized Approach is Key
Deciding whether to proceed with a hair transplant when you have chronic conditions like psoriasis, are taking antidepressants, or have a tendency to form keloids requires a thorough and personalized evaluation. The key to a successful outcome lies in open communication with your medical team. Be prepared to discuss your complete medical history, including all diagnosed conditions and medications, with your hair transplant surgeon and any relevant specialists (like dermatologists). They will assess the specific risks and benefits tailored to your individual circumstances. While these conditions can present challenges, they do not automatically preclude you from receiving a hair transplant. With careful planning, appropriate management, and realistic expectations, many individuals can still achieve satisfactory results. Prioritizing your health and safety throughout the process is paramount, ensuring that the pursuit of restored hair leads to enhanced confidence and well-being.