Considering a hair transplant as a woman can be a significant decision, often stemming from a desire to regain lost confidence and a fuller head of hair. While hair transplantation has become a well-established procedure for men, its application and considerations for women present unique aspects. This article aims to demystify female hair loss and the transplantation process, highlighting what makes it distinct from male procedures.
Key Considerations for Female Hair Loss and Transplantation:
- Understanding the Causes: Female hair loss often has different underlying reasons than male pattern baldness.
- Diagnosis is Crucial: Accurate identification of the hair loss type is paramount for successful treatment.
- Transplantation Techniques: While the core principles are similar, surgical approaches and aesthetic outcomes may differ.
- Donor Area Considerations: The availability and characteristics of the donor hair in women can vary.
- Realistic Expectations: Understanding the potential outcomes and limitations is vital for patient satisfaction.
The Multifaceted Causes of Female Hair Loss
Unlike the typically androgenetic (hormonal) cause of male pattern baldness, female hair loss is frequently more complex and can be attributed to a wider range of factors. Understanding these causes is the first critical step in addressing the issue and determining the most appropriate treatment.
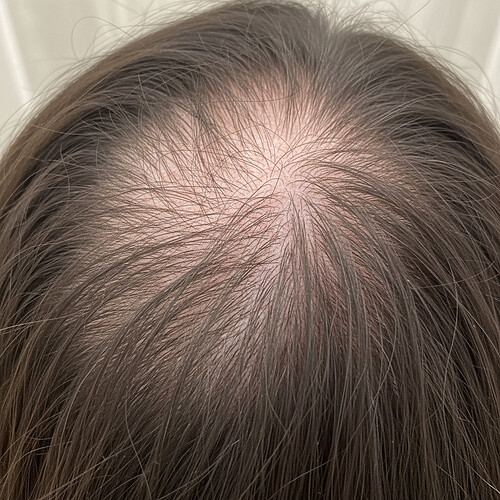
- Androgenetic Alopecia (Female Pattern Hair Loss - FPHL): This is the most common cause, similar to male pattern baldness but presenting differently. Instead of a receding hairline or bald crown, women typically experience diffuse thinning over the top and crown of the scalp, often with the preservation of the frontal hairline. Genetic predisposition and hormonal changes (like those during menopause) play a significant role.
- Telogen Effluvium: This is a temporary form of hair shedding caused by a shock to the system. Triggers can include major surgery, childbirth, significant emotional stress, rapid weight loss, nutritional deficiencies (especially iron, vitamin D, or B vitamins), and certain medications. Hair tends to shed more diffusely across the scalp.
- Alopecia Areata: An autoimmune condition where the immune system mistakenly attacks hair follicles, leading to patchy hair loss. These patches can be small or large, and the condition can sometimes progress to total scalp hair loss (alopecia totalis) or body hair loss (alopecia universalis).
- Traction Alopecia: Caused by persistent pulling on the hair follicles, often due to tight hairstyles like braids, weaves, extensions, or ponytails. It typically affects the hairline and areas where tension is greatest.
- Medical Conditions: Thyroid disorders (both hypothyroidism and hyperthyroidism), polycystic ovary syndrome (PCOS), and scalp infections like ringworm can also lead to hair loss.
- Medications: Certain drugs, including those for blood pressure, heart conditions, depression, and arthritis, can have hair loss as a side effect.
The Importance of Accurate Diagnosis
Before even considering a hair transplant, a thorough diagnosis is essential for women. A dermatologist or a hair loss specialist will typically perform a detailed medical history, examine the scalp, and may conduct blood tests to rule out underlying medical conditions or nutritional deficiencies.
For FPHL, the pattern of thinning is key. For other types, identifying the trigger is crucial. Treating the underlying cause, such as correcting a nutritional deficiency or managing a thyroid issue, can often halt or even reverse hair loss without the need for transplantation. In cases where hair loss has led to permanent follicle damage, transplantation becomes a viable option.
Hair Transplantation for Women: Tailored Approaches
While the fundamental principle of hair transplantation—moving healthy hair follicles from a donor area to a thinning or bald area—remains the same for men and women, the surgical approach, evaluation, and aesthetic goals often differ significantly.
1. Donor Area Considerations:
In men, the donor area (typically the back and sides of the head) is usually abundant and less susceptible to the hormonal influences causing FPHL. For women, the donor area is often evaluated more cautiously. Many women with FPHL have diffuse thinning throughout their scalp, meaning even the ‘donor’ areas might be affected to some degree. This can limit the number of viable grafts that can be safely harvested without compromising the density of the existing hair. Surgeons must be adept at harvesting grafts while maintaining a natural appearance in the donor zone.
2. Surgical Techniques:
- FUT (Follicular Unit Transplantation): This involves removing a thin strip of scalp from the donor area, which is then dissected into individual follicular units (grafts). FUT can yield a high number of grafts but leaves a linear scar. For women, especially those who prefer to wear their hair long, this scar can often be hidden.
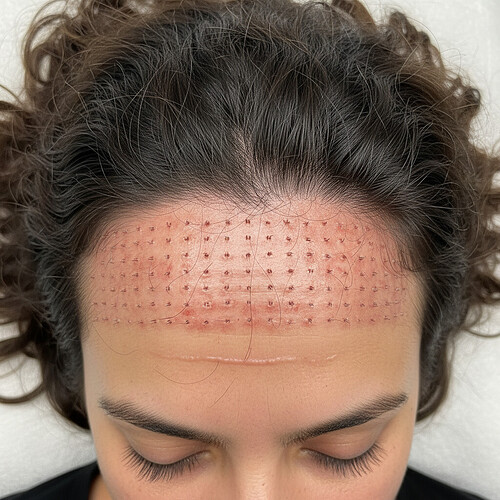
- FUE (Follicular Unit Extraction): This technique involves extracting individual follicular units directly from the donor area using a micro-punch tool. FUE results in tiny, scattered scars that are usually imperceptible, particularly in women with longer hair. It’s often preferred when minimal scarring is a priority or when the donor area is diffuse.
3. Aesthetic Goals and Patterns:
Men typically seek to restore a receding hairline and fill in bald spots on the crown. Women with FPHL often desire increased overall density rather than a drastically altered hairline. The goal is usually to make the existing hair appear fuller and reduce scalp show-through. Therefore, the focus is often on strategically placing grafts to maximize the visual impact of increased density, rather than creating a sharp, defined hairline.
4. Non-Surgical Options:
It’s important for women to explore non-surgical treatments alongside or before considering transplantation. These can include:
- Minoxidil (Rogaine): An over-the-counter topical treatment shown to stimulate hair growth in some women.
- Low-Level Laser Therapy (LLLT): Devices that emit red light to stimulate hair follicles.
- Platelet-Rich Plasma (PRP) Therapy: Involves injecting concentrated platelets from the patient’s own blood into the scalp to promote healing and hair growth.
- Hormonal Therapies: In some cases, prescription medications may be used to address underlying hormonal imbalances.
What to Expect During and After a Female Hair Transplant
A consultation with a qualified surgeon is the first step. They will assess your hair loss pattern, donor density, and overall suitability for transplantation. The procedure itself, whether FUT or FUE, will be performed under local anesthesia with sedation. Post-operative care involves careful attention to the transplanted areas and the donor site to ensure proper healing and optimal graft survival.
Recovery times vary, but most women can return to normal activities within a week or two. Initial shedding of transplanted hairs is normal, with visible growth typically starting around 3-4 months post-procedure and continuing to improve over 12-18 months.
Realistic Expectations are Key
For women, a hair transplant is often about restoring density and improving the appearance of thinning hair, rather than creating a completely new hairline. It’s crucial to have realistic expectations. While transplantation can significantly enhance hair volume and self-esteem, it may not always result in the same dramatic transformation seen in some male procedures. Discussing your goals and concerns openly with your surgeon will help ensure a satisfactory outcome.
In conclusion, while hair transplantation offers a powerful solution for certain types of female hair loss, it requires a nuanced understanding of the diverse causes, careful diagnosis, and tailored surgical approaches. By exploring all options and consulting with experienced specialists, women can make informed decisions to achieve their desired results and regain confidence in their appearance.